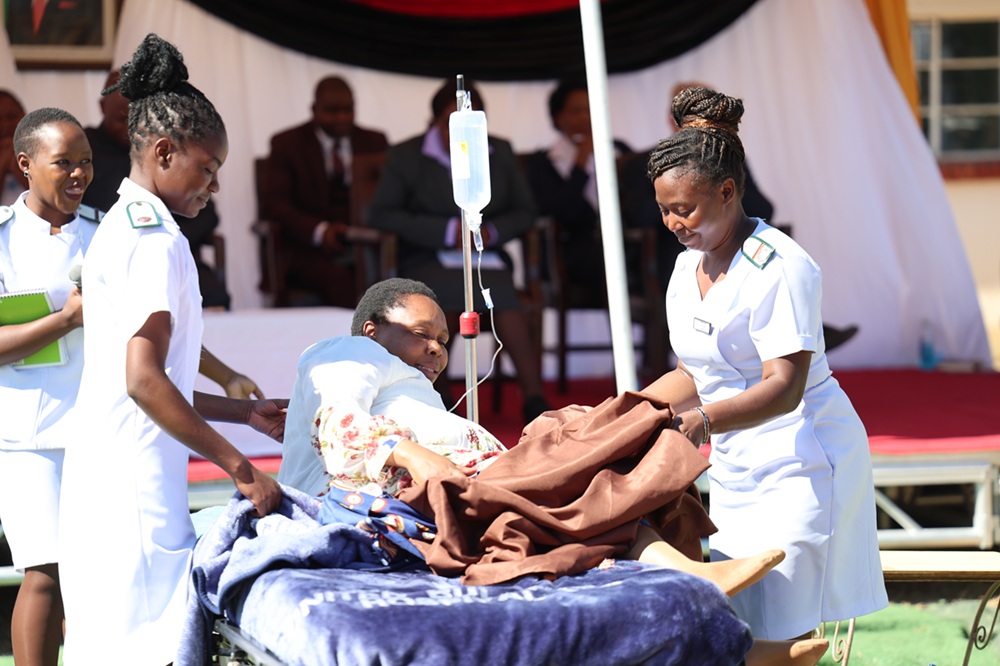
OVER the past few years, Masvingo district has scaled up efforts to increase access to Antiretroviral Therapy (ART) among its citizens. Situated 292 kilometres from the capital Harare, Masvingo is one of the districts performing well in reducing the HIV burden.
By Kudakwashe Pembere
Since 2006, the United States President’s Emergency Plan for AIDS Relief (PEPFAR) has provided over US$650 million to Zimbabwe towards the HIV/AIDS response. Through PEPFAR and the United States Agency for International Development (USAID), a consortium of local partners- Families and Communities for the Elimination of HIV (FACE HIV ), collaborates with the Ministry of Health and Child Care at national, provincial, district and health facility level to support provision of quality HIV care and Treatment services.
Since 2012, the FACE HIV Consortium partners Organisation for Public Health Interventions and Development (OPHID) and J.F KAPNEK Trust, have been at the forefront of advancing comprehensive HIV services, covering 671 health facilities across 24 districts of Zimbabwe.
Owing to combined efforts from health workers and community members, the effort to reduce the ART gap in Masvingo has been tremendous. PEPFAR reports have classified the district as among the 11 districts with a high ART coverage- calculated as the number of individuals receiving ART at a point in time divided by the number of individuals who are eligible to receive treatment at the same point in time (including those who are already receiving ART). Other districts in this category are Mwenezi, Makonde, Chivi, Mutare, Gwanda, Mangwe, Gweru, Beitbridge, Kadoma, Gwanda and Mutare.
According to Masvingo District Nursing officer Sister Georgina Zanga, Masvingo district has a total of 47 health facilities and serves 332, 667 people. The FACE HIV Consortium partner in Masvingo province, JF Kapnek Trust supports 35 health facilities. Through the collaborative efforts, the district has an exceptionally high ART coverage of 99, 3 percent.
“We have a total number of 27, 192 clients on ART and we offer HIV services constituting HIV testing including HIV self-testing, Elimination of Mother to Child Transmission of HIV and Early Infant Diagnosis, HIV Care Services including, provision of ART, Viral Load Monitoring, TB Prevention and Treatment as well as Cervical Cancer Screening- with special focus on Women Living with HIV”, says Sister Zanga.
A visit to Masvingo Provincial Hospital OI Clinic confirmed the facility as a centre of excellence for HIV care and treatment. The facility has eight clinicians with Clemence Ziki as the Nurse in Charge. The Hospital provides all ART and HIV care services under one roof, ensuring that clients do not spend time in winding queues.
Among the HIV Testing Services available at the hospital is index case testing, a strategy that is working well in identifying healthy partners and children who may not be knowing that they are living with HIV (have an undiagnosed HIV infection).
With Index Case Testing, an individual who tests HIV Positive is counselled and advised on the importance of getting their sexual partners and biological children tested for HIV. The individual provides the list of index contacts that will be contacted by the nurses for testing. All ART clients with an unsuppressed viral load (more than 1,000 copies/ml) are also requested to list their sexual contacts for testing, as they are at high risk of HIV infection.
“The goal of index testing is to break the chain of HIV transmission by offering testing to sexual partners and children of persons with a known HIV positive result, and linking them to HIV treatment or prevention services (e.g. VMMC, PrEP, condoms), if HIV negative” says Zanga.
He adds that the nurses always prioritize the safety of clients through assessing and screening for signs of Intimate Partner Violence, as a result of HIV disclosure or request for partner HIV testing. This could be physical, sexual, or psychological harm, including acts of physical aggression, sexual coercion, psychological abuse and controlling behaviors.
If such behaviour is cited, the partners who pose a risk of IPV are excluded from routine partner notification for HIV testing. However, the nurses continue to engage with the index contact and other community systems to find the best way of bringing HIV testing to the sexual partner, while protecting the privacy of the index contact.