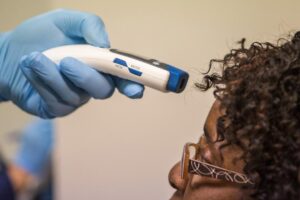
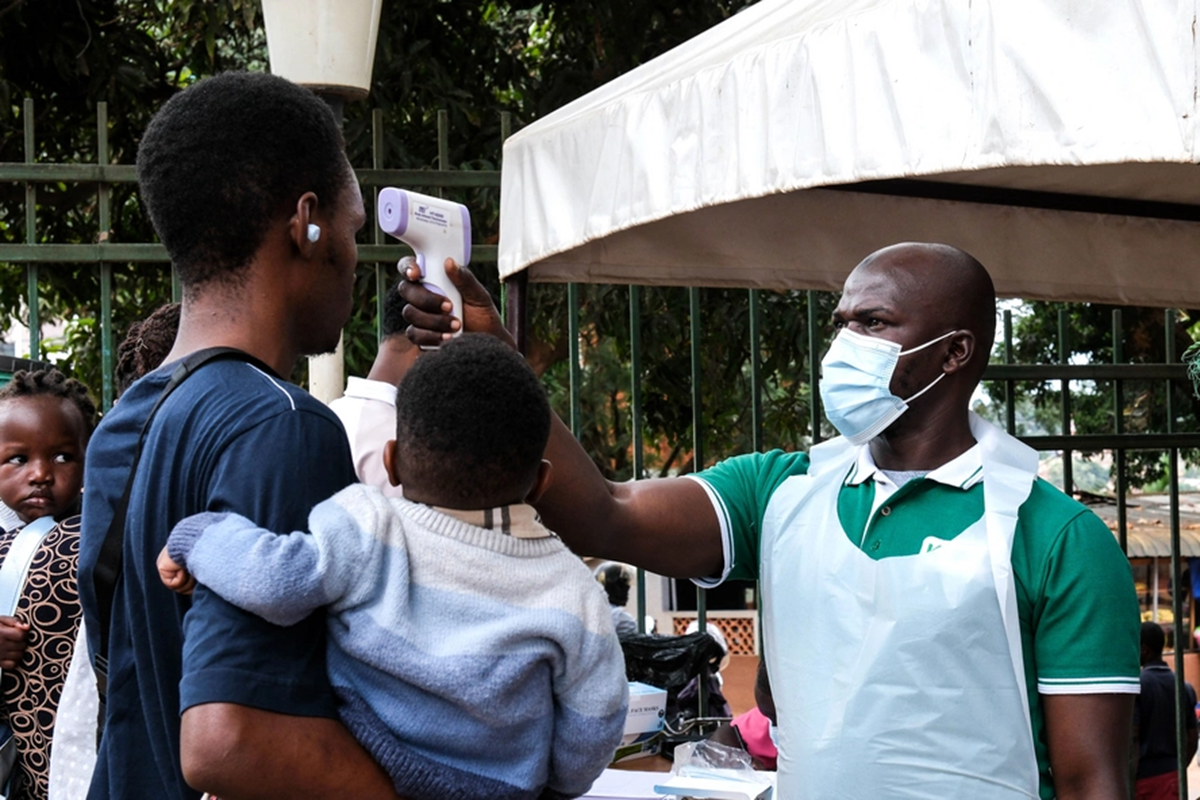
ZIMBABWE and most of Africa are currently in their third wave of the COVID-19 pandemic. Unlike the first two, the current wave has had a very rapid spread across Africa, and also seems to be having a higher fatality rate. Zimbabwe has seen the highest numbers ever reported this week, reporting a record high of over 2600 cases in the past 24 hours, with 55 deaths.
By Dr Grant Murewanhema
There has also been widespread community transmission, with all 10 provinces reporting quite significant numbers of cases. Unlike in the past, other provinces other than Harare, Bulawayo and Manicaland have been severely affected, with Mashonaland West, Mashonaland East and the Midlands reporting hundreds of new cases every day.
The third wave came after a relatively stable period from February to May 2021, where very few daily cases and fatalities were being reported, and the population had largely become complacent to prevention protocols as activities of life were slowly returning to normal. The onset of winter saw the beginning of the third wave, with the cold spell commencing around the last week of May to early January seeing the beginning of the third wave.
Previously, the Indian delta variant which is one of the dominant strains across Africa had been detected in the Midlands, leading to a localised lockdown. Increased human movement, local and international, failure to observe adequate prevention protocols, more transmissible variants such as the delta, and surveillance failures are some of the reasons why we may have had widespread community transmission even before we detected it.
Tobacco sales floors, increased travels to Kariba and Zambia, and increased in-country moved across Mashonaland West possibly resulted in the widespread transmission in that area. The third wave came at a time when Zambia, which had been relatively spared previously, was also seeing the harsh side of the pandemic. Now, South Africa which is usually the African epicenter, has also been reporting massive numbers of new infections, reporting on some days over 20000 new cases.
As the virus continues to spread in Zimbabwe and across Africa, and we lose more people, chances are very high that our public health facilities are slowly becoming overwhelmed and failing to cope with demands for hospitalisation and supportive treatments. The third wave in Zimbabwe is coming at a time when the country is suffering a massive brain drain, having lost thousands of healthcare workers to greener pastures over the past few months. The shortage of consumables and sundries has continued as the hyperinflationary environment continues. Whilst other countries have started seeing marked declines in new cases and fatalities, largely owing to successful mass vaccination campaigns, COVID-19 may in the future remain an African problem.
An urgent intersection of all public health stakeholders is required urgently to find long lasting solutions to the COVID-19 pandemic. We know that governments cannot continue to impose lockdowns on their populations, moreso in countries with very high unemployment rates, where populations live from hand-to-mouth and there is no social support. Children have also been academically affected for quite a while, and school and college activities must be restored to normalcy.
The WHO approved the emergency use of vaccines starting in December 2020. Zimbabwe, though not a part of the COVAX agreement, and had no access to the vaccines that were a part of the arrangement, swiftly moved in to source vaccines from China, India and lately Russia, and remarkably, by the end of the first three months of the programme, had administered over one million doses to its population, with over 600 000 people fully vaccinated. Whilst this is grossly inadequate, we applaud the government for such significant strides, making it a leader among the African countries in terms of COVID-19 vaccination, despite the several economic challenges.
Unfortunately, despite the efforts, the population initially remained largely vaccine hesitant, thanks to successful false information dissemination by influential religious leaders, prominent journalists and other famous members of the society. If we had scrambled for vaccines early enough, there is a possibility the huge demand would have forced the government to increase access and supplies. Whilst vaccines don’t necessarily prevent new infections, studies have continued proving their beneficial effect in terms of reducing hospitalisations, severe disease and death from COVID-19.
This includes results from a huge prospective cohort study published in the New England Journal of Medicine two days ago. All the same, the government has once again made significant strides, securing two million doses of vaccines in the past week. Vaccines are useless in fridges, and effective in people’s arms. We therefore have to accelerate the vaccination programme, to make sure more citizens are protected.
At this point, responsible information dissemination is critical, and is the crux of successful prevention programmes. Religious leaders, prominent journalists and other prominent and trusted people, including healthcare workers, must make sure they are spreading accurate and verified information, including that regarding treatments of COVID-19. There have been false rumours of prophylactic packs circulating directly in the social media, which could give people a false sense of protection from COVID-19, and lead to irresponsible behaviour.
As we move forward, let’s call on all stakeholders involved in public health to make sure that they are educating the public correctly and appropriately, and the Risk Communication and Community Engagement Pillar in the Ministry of Health and Child Care must step up to the challenge. If we are to flatten the curve and reduce mortality from COVID-19, we have to accelerate the dissemination of accurate messages, and upscale our vaccination efforts. Meanwhile, lets educate our people that vaccination will not confer immediate protection, and there is great need to continue observing all prevention protocols as recommended by the WHO and MOHCC.
(Dr Grant Murewanhema, is an Epidemiologist, Public and Reproductive Health Specialist and Obstetrician and Gynaecologist who writes independently in his own capacity. All opinions expressed are personal)