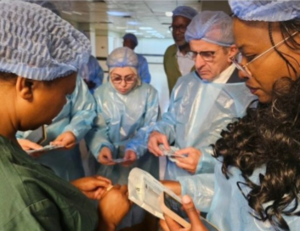
IMPORNTANT advances in COVID-19 research, including data on testing kits and pregnancy, were released today on the third day of the 51st Union World Conference on Lung Health which is being held virtually for the first time. This year’s event includes a special COVID-19 track featuring leading scientists Dr Anthony Fauci, Director of NIAID, Dr Maria Van Kerkhove, Head of the WHO’s Emerging Diseases Unit and epidemiologist Dr Michael T Osterholm.
“The science around COVID-19 is still evolving and there is much we still do not know so it is vital that the Union World Conference assists in addressing questions related to COVID-19 epidemiology, prevention, treatment and care,” said José Luis Castro, Executive Director of the International Union Against Tuberculosis and Lung Disease (The Union), convenor of the Union World Conference and the world`s first global health NGO, which is celebrating its 100th anniversary this year.
As of August 2020, over 21 million COVID-19 cases have been confirmed, however access to timely diagnosis is a persistent challenge world-wide, particularly in the Global South. Commercially available rapid diagnostics that detect SARS-CoV-2 antigens (Ag-RDT) have potential to enable fast and decentralised detection of infection. However, the impact of Ag RDTs depends on their performance and ease-of-use (EoU) at the point-of-care. This study aimed to evaluate six commercially available Ag-RDTs.
A multicentre, prospective study was conducted across COVID-19 testing centres in Brazil, the UK and Germany to assess the clinical accuracy of Ag-RDTs in persons presumed to have COVID-19 compared to routine RT-PCR. All Ag-RDTs were performed using a nasopharyngeal and/or oropharyngeal swab, following the manufacturers’ instructions for use. Results were compared to a draft target product profile developed by the WHO that recommends Ag-RDTs meet minimally 70%/97% and optimally 80%/99% sensitivity and specificity, respectively. Analytical sensitivity was determined using standardized dilutions of the SARS-CoV-2 isolate EMRQ0001/Human/2020/Liverpool propagated in Vero E6 cells.
A System Usability Scale (SUS) questionnaire and EoU assessment were filled by at least 3 operators per test. Jilian Sacks of the Foundation for Innovative New Diagnostics (FIND), reported that clinical performance varied widely: <50%-89% for sensitivity, and 87-100% for specificity. STANDARDQ demonstrated the best overall performance: 76.6%/99.3% sensitivity/specificity in Germany, and 88.7%/97.6% in Brazil. Two tests met the proposed minimal WHO sensitivity target and three met the minimal specificity target. Analytical and clinical sensitivity were consistent, except for Respi-Strip, (albeit with a low sample size). EoU also varied with SUS scores ranging from 54-86 (Table 1).
Sacks noted that the results suggested that though there is substantial variability between tests, at least two Ag-RDTs meet WHO targets. Given the fast turn-around-time and usability at point of contact (POC), these tests are likely to have clinical utility despite imperfect sensitivity, however further research and modelling is needed to assess Ag-RDTs’ impact.
From 966 persons who were screened in the north of Lima for COVID-19, 322 (33%) of 966 persons had a SARV-CoV-2 PCR test positive and 126 (13%) reported to have a cough. From these 126 persons, 2 (1.6%) had Xpert MTB/Rif Ultra positive which means a TB incidence of 1587 per 100000 inhabitants.
Marco Tovar of Partners in Health reported that the implementation of active case finding of TB among people screened for COVID-19 in communities with a high incidence of TB is needed.
Abstract: Tuberculosis and COVID-19 Co-infection among people with cough screened during the active case finding of COVID-19 in community with a high prevalence of tuberculosis (LB-2122-22)
The Washington State COVID-19 in Pregnancy Collaborative was established to identify known pregnant COVID-19 cases from 16 major tertiary referral centres and community hospitals representing >40% of the ~86,000 annual deliveries in Washington State, USA.
Kristina Adams Waldorf reported that the proportion of obese pregnant women in the Washington State COVID-19 in Pregnancy cohort is overrepresented compared to state estimates from the Centers for Disease Control and Prevention.
Waldorf noted that no other co-morbidities or immunocompromised conditions appear to be increased in women with COVID-19.
This study observed 675 women admitted for delivery in New York, 10.4% were positive for SARS-CoV-2, of whom 78.6% were asymptomatic. Caesarean delivery rates were 46.7% in symptomatic COVID-19, 45.5% in asymptomatic COVID-19 and 30.9% in women without COVID-19.
Postpartum complications (fever, hypoxia, readmission) occurred in 12.9% of women with COVID-19 versus 4.5% of women without COVID-19. Among 71 infants tested, none were positive for SARS-CoV-2. Placental pathology demonstrated increased frequency of fetal vascular malperfusion, indicative of thrombi in fetal vessels, in women with COVID-19 versus women without COVID-19 (48.3% versus 11.3%).
Malavika Prabhu of Weill Cornell Medicine reported that among pregnant women with COVID-19 at delivery, the study observed increased caesarean delivery rates and increased frequency of maternal complications in the postpartum period.