Michael Gwarisa, Cape Town
“I almost quit my job so that I could monitor my child,” says Jacky Phillips, the mother of eight-year-old Lorren Hansen, who lives with severe asthma.
Phillips works as a cashier at a fuel station in Atlantis, in South Africa’s Western Cape. She recalls that Lorren’s health challenges began shortly after birth.
“When Loren was born, I noticed red, flared-up skin. Doctors later told us it was eczema,” she says, an early warning sign of an underlying allergic condition.
Today, Lorren is among a growing number of children receiving treatment for chronic respiratory illnesses at the Paediatric Asthma Centre, Red Cross War Memorial Children’s Hospital in Cape Town. Diagnosed with asthma at the age of seven, her condition is classified as severe. Since then, she has been admitted to the intensive care unit twice, highlighting how environmental triggers can provoke life-threatening asthma attacks in vulnerable children. According to her mother, Lorren’s asthma is triggered by exposure to animal fur and dust mites.
Asthma is classified as a chronic respiratory disease and is the most common long-term illness affecting children globally. According to the World Health Organisation (WHO), asthma affects an estimated 339 million people worldwide. Global burden estimates suggest that roughly one in ten children, about 9 to 10 percent, are living with the condition.
Other chronic respiratory diseases commonly affecting children include bronchitis and recurrent lower respiratory infections. These conditions often present with similar symptoms, including wheezing, persistent coughing, shortness of breath, and repeated hospital visits, disrupting schooling, family life, and long-term well-being.
Michael Levin, Professor of Paediatric Allergology at the University of Cape Town and Chief Executive Officer of the Allergy Foundation of South Africa, told journalists that childhood asthma often develops as part of a broader allergic pathway. Speaking during a media workshop organised by PACE University to unpack what experts describe as a growing chronic respiratory disease epidemic, Levin explained that early allergic conditions such as eczema can be the first visible sign of immune dysfunction that later affects the lungs.
“We find that a lower socioeconomic band is associated with asthma and recurrent lung disease, whereas higher socioeconomic bands are associated with allergy, typically inhalant allergies such as rhino conjunctivitis, but also atopic dermatitis (eczema),” said Professor Levin.
Air pollution has also been closely linked to the rising burden of asthma and respiratory infections across sub-Saharan Africa. Exposure to polluted air can trigger asthma attacks in people already living with the condition and increase the risk of developing asthma in the first place, particularly among children, whose lungs are still developing.
Richard van Zyl-Smit, Professor and Consultant Pulmonologist in the Division of Pulmonology at the University of Cape Town and Groote Schuur Hospital, said worsening air quality poses a serious threat to lung health.
“All air pollution contains what we call particulate matter, as well as harmful chemicals. There is no such thing as safe pollution,” he said. “Whether you are walking near a busy road with vehicle emissions, living close to industrial activity, or cooking indoors using wood fires, you are exposed to a combination of particles and chemicals that can cause chronic respiratory disease and even lung cancer.”
Van Zyl-Smit added that other air pollution–related risk factors include toxic fumes from ageing second-hand vehicles imported into the region, rising urban heat, and increased dust exposure—conditions that disproportionately affect children and low-income communities.
While Lorren’s asthma is largely triggered by environmental exposure, not all childhood lung diseases develop in response to surroundings. For some children, chronic respiratory illness begins at birth and is written into their genetic code.
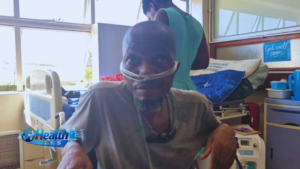
Among them is a young boy, Jolen, who is living with cystic fibrosis—an inherited condition that causes thick mucus to build up in the lungs, leading to recurrent infections and progressive lung damage.
“So my husband and I are just carriers; we do not have cystic fibrosis,” says Ellen-Lee Leitjies, Jolen’s mother. “We never knew about this condition. We only found out when Jolen was six months old.”
At the time, Ellen-Lee was raising Jolen largely on her own following the death of her husband. She recalls losing hope when healthcare workers at the hospital told her that Jolen might not live past the age of 10. Ellen recognized the severity of his condition when Jolen began experiencing persistent shortness of breath, loss of appetite, and other symptoms. She brought him to the hospital, where chest X-rays and other tests confirmed the diagnosis. Jolen was admitted to the intensive care unit multiple times between six months and his first birthday.
Dr. Marco Zampoli, Head of Pulmonology in the Department of Paediatrics at the University of Cape Town and Red Cross War Memorial Children’s Hospital, who also treats Jolen, explained that cystic fibrosis requires lifelong monitoring, medication, and physiotherapy to manage lung infections and maintain health.
“The main manifestation is severe, chronically infected lungs,” said Dr. Zampoli. “Children cough constantly and produce a lot of mucus. It’s a rare chronic condition that requires lifelong care.”
According to Dr. Zampoli, cystic fibrosis affects the pancreas as well as the lungs. In affected babies, mucus blocks the pancreas, preventing digestive enzymes from reaching the gut. As a result, the pancreas essentially “digests itself” from within during fetal development, leaving it unable to produce enough enzymes after birth. This causes severe malnutrition in early life, as children cannot properly digest fats and proteins from milk or food. Over time, the condition also contributes to lung problems. Post-mortem studies of early cases revealed a cystic, fibrotic pancreas that had been damaged from within.
While children like Jolen require lifelong clinical care, public health experts stress that timely prevention and vaccination can protect millions of other children from severe respiratory illness. Dr. Jose Luis Castro, WHO Special Envoy for Chronic Respiratory Diseases and Director of the PACE University Centre for Global Health, told HealthTimes that targeted public health interventions can significantly reduce the burden of these conditions.
“Vaccination is effective in children, and it’s recommended whenever available to ensure that they are protected against conditions that can worsen asthma and other respiratory illnesses. Caregivers should ensure their children are up to date,” said Dr. Castro. Data shows that children who receive routine vaccines—including for flu, pneumococcal infections, and other preventable diseases—are less likely to experience infections that trigger asthma exacerbations, hospitalisations, and emergency visits.