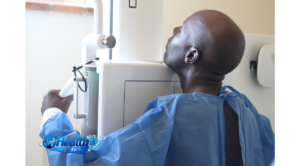
Michael Gwarisa in Kwekwe
A few metres away, the wife of 50-year-old Moses Ndaba stands quietly, her face weighed down by worry as she watches her husband struggle to breathe. Clad in a green dress, she reaches into a plastic bag, pulls out an apple and gently hands it to him. Ndaba stares at it in silence, fully aware that even eating something as simple as an apple can leave him gasping for air.
“I have been admitted at this institution for almost one and a half years and I have never left since,” he says, pausing repeatedly to catch his breath.
Even introducing himself requires immense effort. His weakened lungs fight for every breath as he recounts how years of artisanal mining slowly destroyed his health.
“I worked as a miner because life is difficult. A man has to provide for his family,” he says.
Ndaba is among 18 silicosis patients currently admitted at Kwekwe General Hospital, a facility at the centre of Zimbabwe’s growing occupational health crisis. Once energetic and healthy, he now survives on constant oxygen support.
“A few years ago, I was discharged and went back home. I was given an oxygen cylinder, but I could not power it at home. I became critically ill again and returned to hospital. I only regained consciousness after being connected to oxygen. Since then, I have remained admitted here,” he says.
For patients like Ndaba, electricity is no longer a convenience. It is the thin line between life and death.
Silicosis is a chronic lung disease caused by prolonged inhalation of silica dust, commonly found in mining and construction environments. The disease permanently scars the lungs, making breathing increasingly difficult over time. There is no cure. Treatment focuses on symptom management, oxygen therapy and preventing complications such as tuberculosis.
In Zimbabwe, Midlands Province remains one of the country’s hardest-hit regions due to intensive artisanal and small-scale mining activities. Districts such as Kwekwe, Shurugwi and Zhombe continue to record rising numbers of silicosis cases.
Inside the male ward at Kwekwe General Hospital, the burden of the disease is impossible to ignore. Oxygen concentrators hum continuously beside hospital beds occupied by frail former miners whose lungs can no longer function on their own.
Among them is Sekuru Russell Kambalami, a retired miner who last worked underground more than two decades ago. He spent years blasting rocks in mines, never imagining the dust he inhaled would one day return to haunt him.
“I retired from mining in 2002,” says Kambalami. “Last year, I started struggling to breathe. I went for an X-ray and doctors told me my lungs were filled with fine dust accumulated many years ago while working in the mines.”
The disease progressed rapidly.
“Last week, I tried to stand up from my bed and I collapsed. Now I cannot breathe properly. That is why I was admitted here,” he says.
Hospital authorities say cases like Kambalami’s are becoming increasingly common.
Kwekwe General Hospital Medical Superintendent Dr Tinashe Gunda describes silicosis as one of the district’s biggest public health challenges.
“This is a mining town and many people survive through artisanal mining. Unfortunately, many of them are exposed to silica dust and later develop silicosis,” says Dr Gunda.
“In 2025 alone, we admitted 88 silicosis patients and recorded 42 deaths. This year, we have already admitted around 14 patients. It is a serious burden both for families and for the health system.”
The burden is not only medical. It is also financial.
“These patients rely heavily on oxygen. Oxygen concentrators require electricity to function continuously and oxygen itself is expensive,” says Dr Gunda.
“Every week, the hospital spends between US$1,000 and US$1,500 on medication alone, including steroids and other supportive treatment.”
For years, power cuts posed a major threat to patients dependent on oxygen support. Any prolonged electricity outage meant oxygen concentrators could stop functioning, placing critically ill patients at immediate risk.
Today, however, the situation inside the ward has changed significantly because of a solar energy system installed under Zimbabwe’s COVID-19 Response Mechanism programme, widely known as C19RM.
The solar project, implemented through the Ministry of Health and Child Care with financial support from the Global Fund and technical implementation by the United Nations Development Programme (UNDP), is helping ensure uninterrupted power supply at Kwekwe General Hospital.
Acting Sister-in-Charge Sarah Muhambi says the intervention has transformed care in the silicosis ward.
“In 24 hours, if the ward is full, we can use up to three large oxygen tanks because most of these patients cannot survive without oxygen concentrators,” she explains.
“When electricity goes out, we immediately switch to solar power. This means there is no downtime and patients continue receiving oxygen without interruption.”
She says the solar system has become a critical backup for oxygen delivery systems across the hospital.
“Some patients also rely on piped oxygen from our ICU and HDU sections. The solar system ensures these services continue functioning even during outages,” says Muhambi.
Hospital administrator Abigail Mukazhi says the benefits of solar power extend beyond the silicosis ward.
“The male ward, where many silicosis patients are admitted, has benefited immensely because these patients constantly need oxygen,” says Mukazhi.
“This solar system ensures they do not run out of oxygen at any given time.”
She says several critical departments now rely heavily on solar energy.
“Departments operating on solar include maternity, theatre services and the mortuary. At night, the system becomes even more important because surgeries and emergency cases cannot wait for electricity to return.”
Mukazhi adds that the intervention has also helped reduce operational costs for the hospital.
“It has significantly reduced our electricity bills and improved service delivery. Previously, power outages disrupted essential services, but now we can continue operating critical equipment without interruption.”
The Kwekwe solar project forms part of Zimbabwe’s broader health systems strengthening efforts under the Global Fund’s COVID-19 Response Mechanism.
Since 2020, Zimbabwe has received more than US$180 million under the C19RM programme to support both the COVID-19 response and long-term health system improvements.
Approximately US$51 million of the funding has been managed by UNDP, focusing largely on infrastructure development, including solar energy systems, water supply improvements, diagnostic equipment, pharmaceutical storage and healthcare waste management systems. The remaining funds have been implemented by the Ministry of Health and Child Care.
Although initially mobilised in response to the COVID-19 pandemic, many of the investments are now addressing long-standing weaknesses within Zimbabwe’s healthcare system.
At Kwekwe General Hospital, the impact is visible not only in infrastructure, but also in human survival.
For patients battling advanced silicosis, uninterrupted electricity means oxygen concentrators continue working through the night. It means doctors can respond to emergencies without delays. It means families no longer panic every time power cuts hit the town.
For Ndaba, whose life now revolves around oxygen tubes and hospital walls, the solar system has become something deeply personal.
Without it, survival would be uncertain.
As the afternoon sun settles over Kwekwe General Hospital, the soft hum of oxygen concentrators continues inside the ward. Beside Ndaba, his wife remains seated quietly, watching over him.
He slowly lifts the apple she handed him earlier. Then he pauses again to breathe.