By Kuda Pembere
The Association of Healthcare Funders of Zimbabwe (AHFoZ) is convinced that healthcare funders could be losing more than US$500 000 every quarter on the back of fraudulent claims made by some cartels in the health sector.
The funds recovered in 2022, a period in which healthcare fund members collectively paid more than US$164 million towards settlements of claims by clients.
In some cases, corrupt syndicates involving pharmacists and doctors would generate fraudulent medical aid claims and receive money for services not rendered
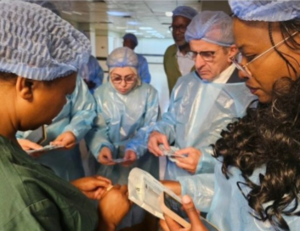
AHFoZ board chair Mr Stanford Sisya told HealthTimes on the sidelines of the organization’s annual Fraud Indaba held in Harare.
He said the triple threat of fraud, waste and misuse and abuse bleed medical aid companies over 30 percent of its revenue.
“We have had our AHFoZ annual fraud indaba, which we actually hold every year. It’s one of the key events in our calendar. One to encourage sharing of ideas, collaboration among the providers and all the stakeholders across be it the police, the regulators, the players in the industry.
“One of the things that we have noted is that fraud, waste and abuse are the biggest evils in our industry, whereby we are actually looking at as high as up to 30 to 35 percent of revenues lost through those three evils,” Mr Sisya said.
Mr Sisya added that fraudulent claims are rampant to an extent where the figure could surpass US$500 000.
“So when you look at AHFoZ we actually, on a quarterly basis, we are actually recovering almost close to a minimum of half a million dollars per quarter of fraudulent claims that would have picked as an industry, but we believe that it’s actually bigger than that,” he said.
He said going digital is the way to go to pick up these practices. Mr Sisya noted that there are cartels colluding to over-service medical funders.
“So when you look at AHFoZ we actually, on a quarterly basis, we are actually covering almost close to a minimum of half a million dollars per quarter of fraudulent claims that would have picked as an industry, but we believe that it’s actually bigger than that.
“So we are also encouraging our members also to go digital to ensure that we actually pick on these bad practices that are happening in the industry.
“When you look at it, some of the issues that come up is issues of over-servicing, where people don’t actually need that particular service, but there are always cartels whereby actually people collaborate and collude to actually over service a client and they offer them services that they don’t need.
“I think we’ve had delegates sharing what they experienced whereby even the specialist didn’t attend to them, but the specialist office actually requested that they should come through and complete a claim, which was not proper,” Mr Sisya noted.
From South Africa, Dr Hleli Nhlapo, chairperson of the Board of Healthcare Funders (BHF) Healthcare Forensic Management Unit (HFMU) said collaboration is the panacea to deal with fraud within the healthcare funding space.
“Collaboration, collaboration, collaboration. We found that when you collaborate as an industry there’s more gains than loss in that arrangement because information gets shared. As a funder, if you’re just looking at your claims, you may not see a bigger picture of what other funders are experiencing.
“You might think you are the only one that is experiencing a problem with a service provider, only to find that everyone is having the same issues, but because you are not talking to each other, you don’t find that, you won’t be aware of that.
“But once you collaborate, you work together, like in South Africa we’ve got a portal within PHF that the HFMU uses to log suspicious cases and things like that and it’s shared amongst the industry. That helps,” he said.