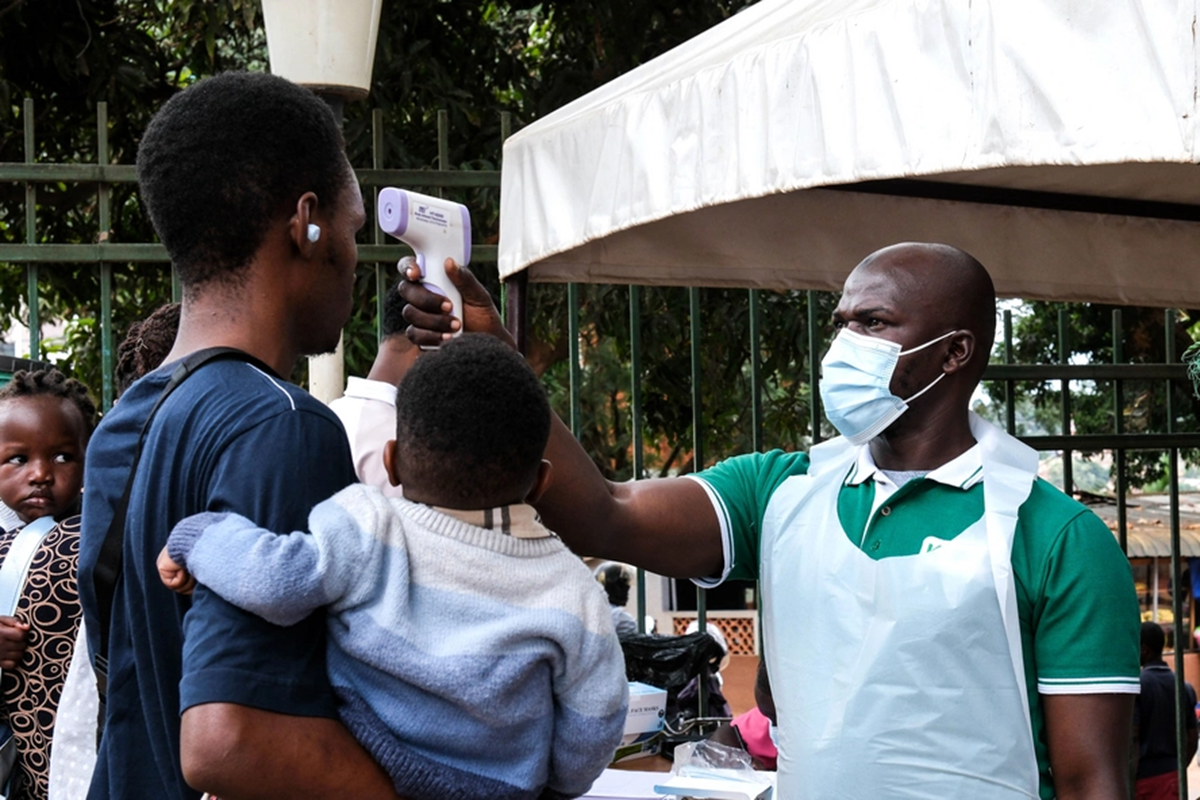
In Zimbabwe, a host of barriers are preventing adolescents, defined as aged 10 to 19 years, from accessing sexual and reproductive health (SRH) services safely and confidentially without the consent of their parents.
HealthTimes Reporter
Without free and informative access to health services that include contraceptives, treatment for sexually transmitted infections and condoms, national studies show that rates of adolescent pregnancy and HIV are increasing, while knowledge levels around sexual health are declining. One study revealed that Zimbabwe has the highest teenage fertility rate in sub-Saharan Africa with one in every 10 girls aged between 15 and 19 years falling pregnant every year.
Culturally, young people are often expected to abstain from sex until they get married. National law states that young people below the age of 16 years can’t take an HIV test without parental consent, and health workers often stigmatize young people seeking sexual health advice.
Yet in many communities like Mbare, a sprawling high-density suburb in the capital Harare, the reality is that young people start having sex and experimenting as early as 12 years, frequently without protection or information on how to prevent unwanted pregnancies, STIs and HIV infection.
Young people living with HIV also face particular difficulties, especially if they only learn of their HIV status by accident in their teens. Most find it difficult to accept their condition, and often stop taking their antiretroviral treatment (ART). Crowded living conditions which force young people out of their homes and abuse of alcohol and drugs also plays havoc with staying on regular treatment.
Recognizing the huge vulnerability of adolescents without access to free sexual and reproductive health services, MSF partnered with the Harare City health department to start an ‘adolescent-friendly corner’ at Edith Opperman clinic in Mbare. Staff in the brightly coloured rooms offer free services which include general health check-ups, HIV testing and counselling, screening for sexually transmitted infections (STIs) and contraceptive services.
In between appointments, young visitors can play pool or chat with ‘peer educators’, themselves young people, who MSF has trained and mentored to discuss sexual health issues with their peers or encourage them to stick to their treatment.
In 2017, 2454 consultations were provided for young people in the ‘adolescent corner.